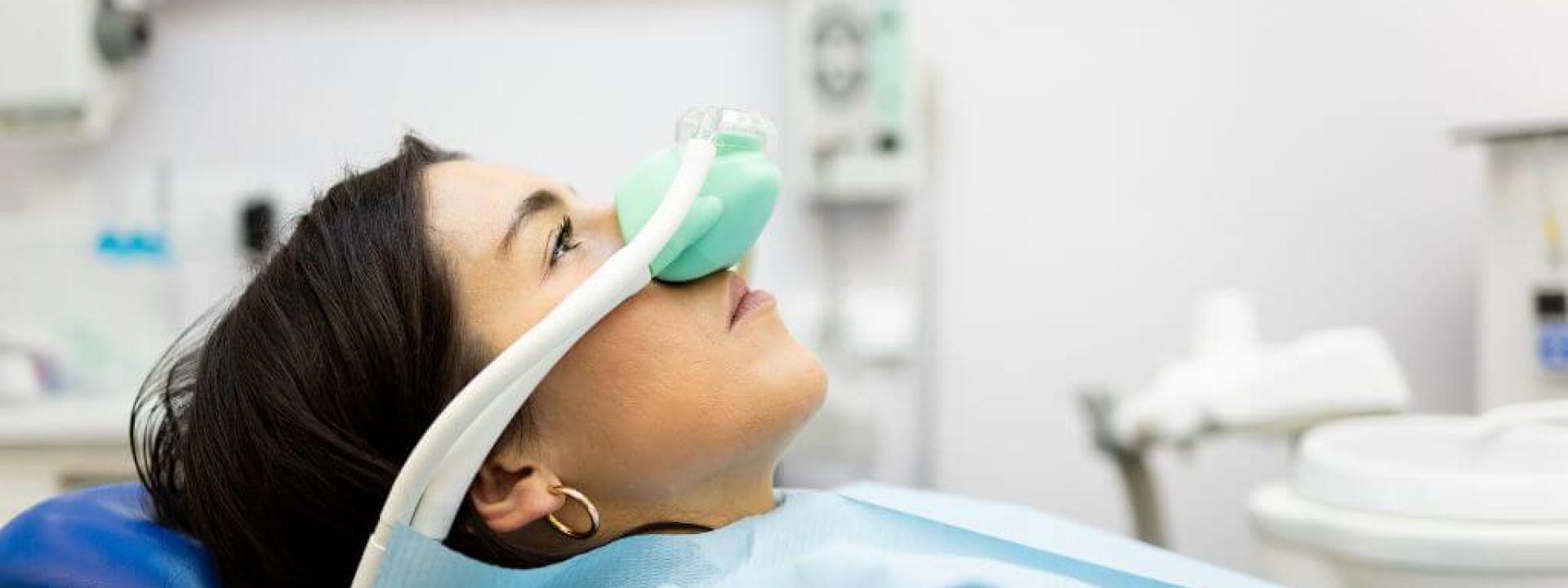
Oral surgery is a common and often necessary part of maintaining your oral health. Still, it is completely normal to feel nervous about anesthesia and sedation. Many patients want to know what their options are, how safe those options are, and what to expect before and after the procedure. Clear information can go a long way toward easing anxiety and helping you feel confident about your care.
Whether you are planning for a tooth extraction, dental implant placement, or another oral surgical procedure, understanding how anesthesia works and how your oral surgeon keeps you safe can help you make informed decisions. Below are answers to common questions about anesthesia and oral surgery.
Anesthesia Options for Oral Surgery: What Are Your Choices?
Not every procedure requires the same type of anesthesia. The right option depends on the complexity of your surgery, your medical history, and your comfort level. Your oral surgeon will review your health background and discuss which form of anesthesia is appropriate for you.
Local anesthesia is the most common option for many minor surgical procedures. A numbing medication is injected near the treatment area so you remain fully awake but do not feel pain in that specific region. You may still feel pressure, but sharp discomfort is typically blocked.
Types of Sedation Used in Oral Surgery
For patients who feel anxious or who are undergoing more involved procedures, additional sedation options may be recommended. These can include:
- Nitrous oxide (laughing gas): Inhaled through a mask, nitrous oxide helps you feel relaxed during treatment. Its effects wear off quickly once the gas is stopped, and many patients can return to normal activities soon after.
- Oral conscious sedation: A prescribed medication taken before the procedure helps reduce anxiety and promote relaxation. You will remain responsive but may feel drowsy. Because the effects can linger, you will need someone to drive you home.
- IV sedation: Medication is delivered through a vein to produce a deeper level of relaxation. Patients often have little memory of the procedure. Close monitoring is required throughout treatment.
- General anesthesia: Used for certain complex procedures or specific medical situations, general anesthesia renders you fully unconscious. This level of anesthesia requires advanced training and strict monitoring protocols.
Each of these methods has specific indications and safety requirements. Your surgeon will tailor the plan to your needs while prioritizing your overall health and safety.
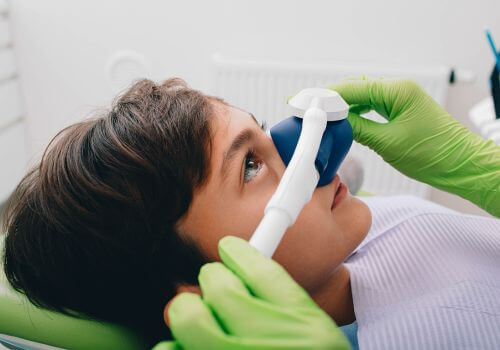
How Safe Is Anesthesia in Oral Surgery?
Patient safety is the top priority in any surgical setting. Oral and maxillofacial surgeons receive hospital-based training in anesthesia as part of their specialty education. This includes experience in airway management, emergency response, and patient monitoring.
Board-certified oral and maxillofacial surgeons complete rigorous training and examinations through the American Board of Oral and Maxillofacial Surgery. This certification reflects advanced education in both surgery and anesthesia administration.
During sedation or general anesthesia, your vital signs are continuously monitored. This typically includes heart rate, blood pressure, oxygen saturation, and breathing rate. Monitoring standards are consistent with established surgical safety guidelines. Offices that provide moderate-to-deep sedation or general anesthesia are also required to maintain emergency equipment and medications.
Anesthesia complications are uncommon in healthy individuals when proper screening and monitoring are in place. Before your procedure, you will be asked detailed questions about your medical history, medications, allergies, and prior experiences with anesthesia. This information helps your surgeon determine the safest approach for you.
How to Prepare for Oral Surgery With Anesthesia
Preparation instructions vary depending on the type of anesthesia being used. If you are receiving moderate-to-deep sedation or general anesthesia, you will likely be asked to avoid eating or drinking for a specific period before your appointment. Fasting helps reduce the risk of nausea and aspiration during sedation.
In many cases, patients are instructed not to eat solid food for at least eight hours before surgery and to avoid clear liquids for a shorter window prior to treatment. However, exact instructions may vary depending on your health status and the planned anesthesia. Always follow the personalized directions provided by your surgical team.
You should also:
- Arrange for a responsible adult to drive you to and from the appointment if you are receiving oral sedation, IV sedation, or general anesthesia.
- Wear comfortable clothing with short sleeves to allow access for monitoring equipment.
- Review your medication list with the office, including over-the-counter supplements.
If you have conditions such as heart disease, diabetes, or respiratory concerns, your surgeon may coordinate with your primary care physician or specialist before proceeding.
Will I Need Someone to Drive Me Home?
Transportation requirements depend on the level of sedation used. With nitrous oxide alone, the effects typically resolve quickly after the mask is removed. Many patients feel alert enough to drive themselves home, although individual responses can vary.
If you receive oral sedation, IV sedation, or general anesthesia, you should not drive, operate machinery, or make important decisions for the rest of the day. These medications can affect coordination, judgment, and reaction time, even if you feel awake. A trusted adult should accompany you to the appointment, remain on site during the procedure, and drive you home afterward.
Planning transportation in advance helps your recovery begin smoothly and safely.
Is the Surgical Team Prepared for Anesthesia Emergencies?
Although anesthesia emergencies are rare, preparation is essential. Oral surgery teams are trained in basic and advanced life support. Emergency protocols are rehearsed regularly so that each team member understands their role.
Surgical offices that provide sedation and general anesthesia maintain emergency medications, oxygen, airway equipment, and monitoring devices. These safeguards are part of standard-of-care practice in oral and maxillofacial surgery settings.
Before your procedure, do not hesitate to ask about your surgeon’s training, the credentials of the team, and the safety measures in place. Open communication is encouraged and can provide additional reassurance.
Making an Informed Decision About Sedation Dentistry
Choosing to move forward with oral surgery is often an important step toward protecting your long-term oral health. When you understand your anesthesia options and what to expect, the experience can feel much more manageable.
If you are unsure which level of sedation is right for you, schedule a consultation to review your medical history, discuss your concerns, and ask questions. Your comfort matters, and a personalized plan can help ensure that your procedure is both safe and as stress-free as possible.
Clear information, proper preparation, and a trained surgical team all work together to support a positive experience. With the right approach, oral surgery and anesthesia can be handled safely and confidently.
If you have questions, we would love to answer them for you. Please give us a call at the office at (931) 277-4666, or you can email us at [email protected]. Our staff would love to talk with you!